Targeting PD-L1
Indication: Pancreatic cancer, NSCL, melanoma and breast cancer
- Checkpoint Inhibitor targeting PD-L1
- Multiple cancer types
- Advantages over other checkpoint inhibitors
PD-L1 Expression as a Predictive Biomarker in Cancer Immunotherapy:
- The resurgence of cancer immunotherapy stems from an improved understanding of the tumor microenvironment.
- PD-1/PD-L1 - demonstrates a restoration of host immunity in multiple human cancers, generating durable responses and extended overall survival. Clinical responses have been seen in several different malignancies including, but not limited to, melanoma, lung, kidney, and bladder cancers. However, Pancreatic cancer has proven difficult to treat with conventional drugs and has been resistant to initial immunotherapy approaches due to:
- Complex tumor microenvironment that characterizes pancreatic adenocarcinoma.
- Presence of desmoplastic tumor stroma that is both immunosuppressive in nature and a physical barrier for antibody and T lymphocytes infiltration.
- Consequently, it is important to design an efficient delivery mechanism to tumor cells and tumor resident macrophages, and strategies that enhance the permeation of the tumor by T lymphocytes. With our therapeutic approach we expect to prevent the synthesis of PD-L1 all together rather than blocking its function. Because TTX-siPDL1 incorporates a siRNA against PD-L1 as its functional component, it inactivates PD-L1 at the post-transcriptional level, that is, it triggers the degradation and/or translational repression of the PD-L1 messenger RNA (mRNA), preventing the cell from expressing the PD-L1 antigen.
- Since we are utilizing an RNAi approach our therapeutic has the potential to be more efficient, which could result in increased efficiency for T cells to recognize and kill tumor cells.
- The RNA mechanism has been shown to be catalytic and has been observed in in vitro studies to necessitate the delivery of only picomolar amounts of siRNA to the tumor cell for the abolition of the target antigen.
Pre-clinical Results:
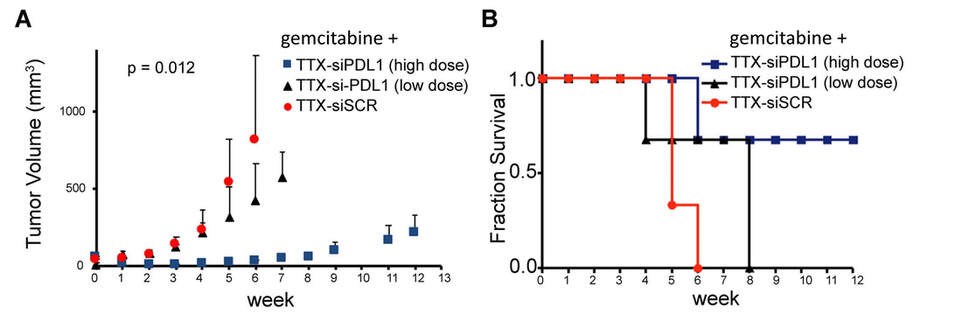
TTX-siPDL1 - Robust Therapeutic Response
In animal models of PDAC,
- High-dose TTX-siPDL1 + gemcitabine regressed pancreatic tumors by 90% within the first two weeks of treatment and delayed tumor growth (Figure A above).
- Treatment increased survival - 67% of the experimental animals survived for 12 weeks (Figure B above).